Closing the medicine gap: Improving First Nations peoples’ access to medicine
Closing the medicine gap: Improving First Nations peoples’ access to medicine
While several programs, such as Closing the Gap PBS co-payment are in place, obstacles such as geographic isolation, high costs and insufficient culturally safe care services persist. These challenges hinder access to safe and efficacious treatments.
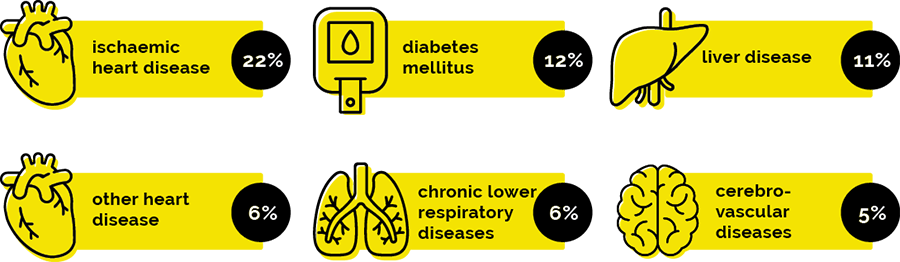
First Nations people experience higher rates of chronic disease than other Australians. These conditions, such as diabetes and heart disease, are more common leading to greater burden of illness, disability, and even early death. In fact, chronic diseases account for a staggering 80 per cent of the life expectancy gap between First Nations people and the rest of the population. Tragically, medicines are readily available in Australia to manage these conditions.
Practical recommendations for change
To bridge this gap, our report suggests several actionable steps:
Amplify First Nations voice in the PBAC process
Giving First Nations people the opportunity to advise on health matters that impact them will contribute to better
Embed culturally safe care in ACCHOs
We know that empowering First Nations people to take control of their health is essential for improving health outcomes, this includes embedded pharmacists and expanding the role of Aboriginal and Torres Strait Islander Health Workers (ATSIHW) in Aboriginal Community Controlled Health Organisations (ACCHOs).
Unlock access through PBAC fee waivers
We propose automatic fee waivers for any application related to Aboriginal and Torres Strait Islander health. Additionally, government-provided assistance with writing these submissions would empower these communities to advocate for their specific health needs.
Expand the PBS Prescribers Bag
Expanding the Prescribers Bag program would equip ACCHOs to hold and dispense PBS-funded medications directly to their patients.

Renae Beardmore
Managing Director, Evohealth





